Last Updated on June 16, 2023 by Admin

You are participating in the customization and implementation of a barcode medication administration system. In a 500-word APA essay, analyze how the process flow will change from the current manual process to a barcode process and identify potential problem areas and possible solutions. Additionally, include a workflow diagram (Process Flowchart) from the manual process to the barcode process.
The resources to get started on this project are in the Additional Resources for this module.
Assignment Expectations
Length: 500 words; answers must thoroughly address the questions in a clear, concise manner.
Structure: Include a title page and reference page in APA style. These do not count towards the minimum word count for this assignment.
References: Use the appropriate APA style in-text citations and references for all resources utilized to answer the questions. Include at least three (3) scholarly sources to support your claims.
Format: Save your assignment as a Microsoft Word document (.doc or .docx).
File name: Name your saved file according to your first initial, last name, and the assignment number (for example, “RHall Assignment 1.docx”)
Expert Answer and Explanation
The Customization and Implementation of a Barcode Medication Administration System
Healthcare barcode solutions are vital when it comes to providing safe and quality data. Wilson et al. (2020) note that barcode solutions help track patient medication, modernize the patient admission procedure, track patient admission, and identify the clients when they are in hospital. The barcode system can also reduce medical errors by ensuring that the nurses administer the right medication. The purpose of this assignment is to analyze how my organization’s flow process with the transition from the current manual to a barcode process, and identify the potential problem areas and solutions.
Analysis of The Current Process
The current process is a manual process where information is processed manually. The majority of the activities are done manually with paper and pen. For instance, when a patient enters the hospital, they will be admitted manually and their names entered into the system using pen and paper (Samadbeik et al., 2017). Also, in the current process, the input is collected in a tray and the person in charge is required to apply their brain to reply to the inquiries.
This type of data management can encourage medical errors, especially when the person making data entry is exhausted or tired. For instance, the nurse at the admission point can mistype the name of the patient, hence leading to a medication administration error. Patient privacy can also be breached if data in the “tray” or the file cabinet is accessed by unauthorized individuals. Manual data management is tiring because it involves repeating the same process many times.
Manual data processing also takes too much space (McGonigle & Mastrian, 2017). Hospitals applying this process need a huge scape to design file cabinets that can be used to store data. Information in manual data processing can easily be lost or damaged. Making changes to data created by hand is hard and this can create a lot of inconveniences.
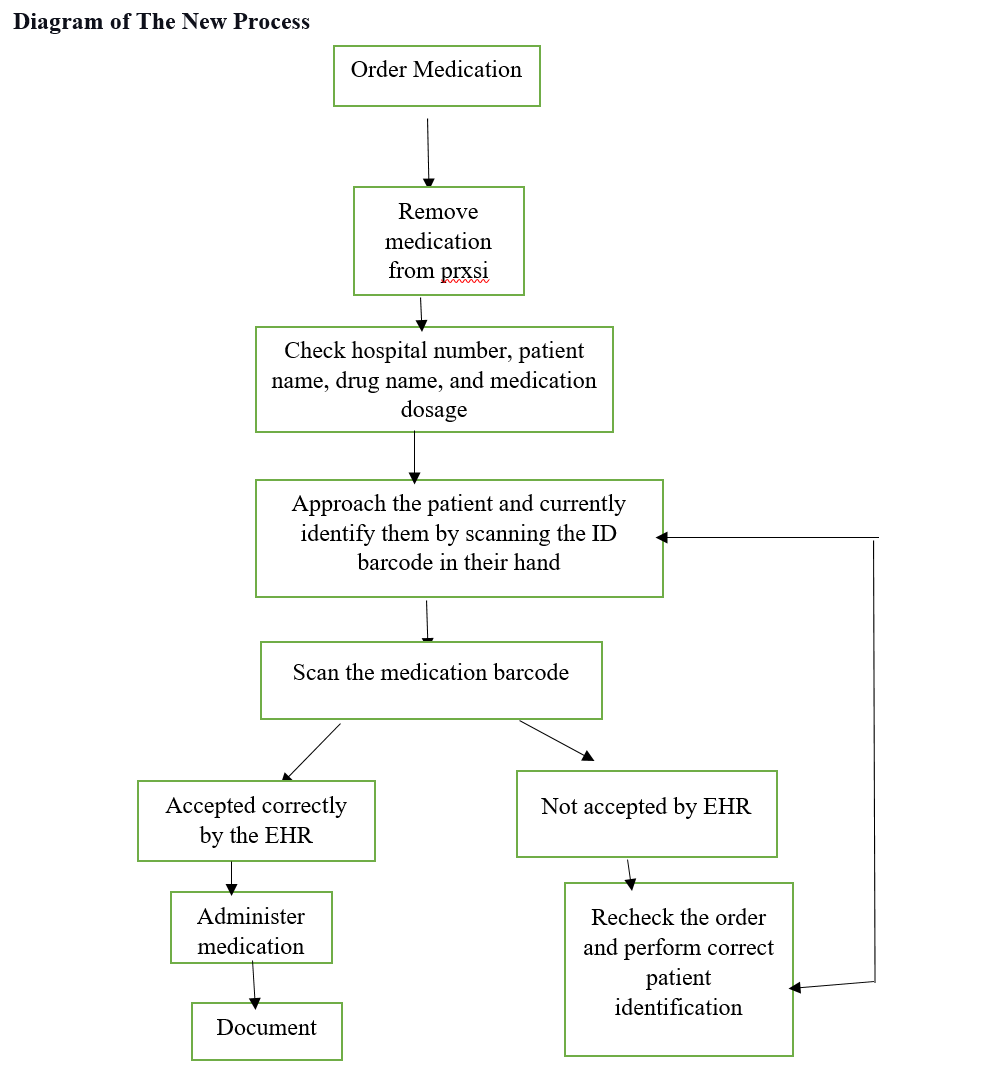
Discussion of The New Process
Healthcare professionals have been developing electronic data management systems to solve the flaws in the manual data processing system. Barcode system that solves most of the flaws experienced in manual data processing. As seen in the diagram above, the barcode system can help a nurse determine whether the medication provided by the pharmacists is indeed prescribed to a specific patient, hence preventing prescription error (McGonigle & Mastrian, 2017).
In the diagram, if the medication does not match the patient barcode, then the drugs will be returned and the correct order made. The barcode system can also solve the issue of space because all the data will be stored on the computer hardware. In some situations, data can be stored in a cloudscape. Barcode data processing can also improve the time where the patient can get care. The barcode process can cause various problems in healthcare. One of the issues is that nurses can lose creativity because of the overdependence of electronic systems to perform nursing services (Jimenez, 2017). This problem can be solved by exposing nurses to constant training and education to improve their knowledge and skills.
Conclusion
Barcode data can improve care by reducing time for accessing care, improving quality and safety of care by reducing medical errors, and improve the safety of patient data.
References
Jimenez, M. (2017). Effects of Barcode Medication Administration: Literature Review. Proceedings of the Northeast Business & Economics Association. http://web.a.ebscohost.com/ehost/detail/detail?vid=0&sid=94e40e24-1d39-4b2e-b98e-1f88c6267265%40sdc-v-sessmgr01&bdata=JnNpdGU9ZWhvc3QtbGl2ZQ%3d%3d#AN=134235278&db=bth
McGonigle, D., & Mastrian, K. (2017). Nursing Informatics and the Foundation of Knowledge (4th ed.). Jones & Bartlett Learning. ISBN: 978-1284121247.
Samadbeik, M., Shahrokhi, N., Saremian, M., Garavand, A., & Birjandi, M. (2017). Information processing in nursing information systems: An evaluation study from a developing country. Iranian Journal of Nursing and Midwifery Research, 22(5), 377. doi: 10.4103/ijnmr.IJNMR_201_16
Wilson, N., Jehn, M., Kisana, H., Reimer, D., Meister, D., Valentine, K., … & Clarke, H. (2020). Nurses’ perceptions of implant barcode scanning in surgical services. CIN: Computers, Informatics, Nursing, 38(3), 131-138. doi: 10.1097/CIN.0000000000000579
Place your order now for the similar assignment and get fast, cheap and best quality work written by our expert level assignment writers.
Use Coupon Code: NEW30 to Get 30% OFF Your First Order
Answered Questions:
[ANSWERED] Identify a quality improvement opportunity in
[ANSWERED] Develop an interview questionnaire to be used in a family-focused functional assessment
[ANSWERED] Select a family, other than your own, and seek
ANSWERED! In this project you will select an organization or
[ANSWERED] What is the significance of the product lifecycle
ANSWERED! How can different types of attributions and
ANSWERED!! Lily is a 20-year-old student at
ANSWERED!! In 4 or 5 sentences describe the anatomy of the basic unit of the nervous system
barcode medication administration, barcoding medication administration, medication barcodes, medication barcode, medication barcode scanningmedication barcode scanning, barcode scanning medication administration, medication administration systems, barcode medication administration benefits
Bar Code Medication Administration: Enhancing Patient Safety and Medication Management
Introduction
In today’s fast-paced healthcare environment, patient safety is of paramount importance. One critical aspect of patient safety is the accurate administration of medications. Bar Code Medication Administration (BCMA) has emerged as a powerful tool to enhance patient safety, reduce medication errors, and improve medication management in healthcare settings. This article explores the concept of BCMA, its benefits, implementation considerations, and its impact on patient outcomes.
What is Bar Code Medication Administration (BCMA)?
Bar Code Medication Administration (BCMA) is a technology-driven system that employs barcodes to ensure the accurate and safe administration of medications to patients in healthcare settings. BCMA involves the use of barcodes on medication packaging, patient identification wristbands, and healthcare professionals’ identification badges. By scanning these barcodes at various points along the medication administration process, BCMA verifies the right medication, right dose, right route, and right patient, thus minimizing the risk of medication errors.
The Benefits of BCMA
BCMA offers several benefits in improving patient safety and medication management:
- Reduced Medication Errors: BCMA significantly reduces medication errors by matching the medication and patient data with the electronic medication administration record (eMAR) in real-time. It helps prevent medication administration errors such as wrong medication, wrong dose, wrong patient, or wrong route.
- Enhanced Patient Safety: With BCMA, healthcare providers can be confident that the right medication is being administered to the right patient at the right time, significantly reducing adverse drug events and improving patient outcomes.
- Real-Time Documentation: BCMA enables accurate and real-time documentation of medication administration, enhancing the completeness and accuracy of patient records. This documentation aids in medication reconciliation and provides valuable data for quality improvement initiatives.
- Clinical Decision Support: BCMA systems can be integrated with clinical decision support tools, providing healthcare professionals with alerts, reminders, and drug interaction warnings at the point of care. This functionality enhances medication safety and supports evidence-based practice.
Implementation of BCMA
Successful implementation of BCMA requires careful planning, coordination, and consideration of various factors. The following elements are crucial for a smooth BCMA implementation:
Bar Code Technology
BCMA relies on barcodes for accurate identification and tracking of medications, patients, and healthcare providers. It is essential to have a reliable barcode scanning infrastructure and ensure the standardization of barcode symbologies and formats.
Integration with Electronic Health Records (EHRs)
Seamless integration of BCMA with electronic health records (EHRs) is vital to access real-time patient information, medication orders, and allergy alerts. Integration eliminates the need for manual data entry and enables automatic documentation of medication administration.
Staff Training and Workflow Adaptation
Successful BCMA implementation necessitates comprehensive training programs for healthcare professionals. Staff members should be educated on the proper use of barcode scanners, workflow changes, and the importance of adhering to BCMA protocols. Workflow processes may need to be adapted to incorporate BCMA effectively.
Enhancing Medication Safety through BCMA
Verification of Medication and Patient Identity
BCMA ensures accurate medication administration by verifying the medication and patient identity using barcode scanning. It reduces the risk of medication errors caused by look-alike or sound-alike medications and misidentification of patients.
Reducing Medication Errors
BCMA significantly reduces medication errors by alerting healthcare professionals in case of discrepancies between the prescribed medication and the scanned barcode. It promotes double-checking and validation, enhancing medication safety.
Real-Time Documentation
By documenting medication administration in real-time, BCMA provides accurate and up-to-date information for healthcare providers. This documentation aids in medication reconciliation, reduces documentation errors, and supports comprehensive patient care.
Decision Support and Clinical Alerts
BCMA systems can be integrated with clinical decision support tools to provide alerts for potential drug interactions, allergies, or contraindications. These alerts improve medication safety by guiding healthcare professionals in making informed decisions.
Considerations for Successful BCMA Implementation
Implementing BCMA successfully requires addressing the following considerations:
System Integration and Interoperability
BCMA systems should integrate seamlessly with existing healthcare technologies, including EHRs, pharmacy information systems, and computerized provider order entry (CPOE) systems. Interoperability ensures efficient data exchange and supports a cohesive medication management process.
Barcode Scanning Infrastructure
A robust and reliable barcode scanning infrastructure is critical for BCMA implementation. Barcode scanners should be easily accessible, properly maintained, and capable of scanning various barcode formats commonly used in healthcare settings.
Standardization of Medication Packaging
Standardizing medication packaging with clear and scannable barcodes improves the accuracy and efficiency of BCMA. Consistent barcode formats and symbologies across medication manufacturers facilitate the scanning process and reduce the risk of errors.
Staff Buy-In and Training
Successful BCMA implementation requires the engagement and support of healthcare professionals. Adequate training programs should be provided to ensure that staff members are comfortable and proficient in using the BCMA system. Ongoing education and support are essential for sustained success.
Challenges and Limitations of BCMA
While BCMA offers significant benefits, it also poses certain challenges and limitations:
- Initial implementation costs and infrastructure requirements can be substantial, including barcode scanners, software systems, and system integration.
- Technical issues such as barcode scanning failures or system downtime can impact workflow efficiency and potentially compromise patient safety.
- Staff resistance or reluctance to adopt new technology and workflow changes can hinder the successful implementation and utilization of BCMA.
- Barcode-related challenges, such as damaged or illegible barcodes, require processes for managing exceptions and ensuring medication safety.
Future Trends and Innovations in BCMA
The field of BCMA continues to evolve, with ongoing advancements and innovations. Some future trends include:
- Mobile BCMA solutions that leverage smartphones or handheld devices for barcode scanning, improving accessibility and workflow flexibility.
- Integration of BCMA with emerging technologies such as artificial intelligence (AI) and machine learning to enhance medication safety and personalize patient care.
- Continued refinement of barcode standards and symbologies to ensure interoperability and optimize scanning accuracy.
Conclusion
Bar Code Medication Administration (BCMA) is a powerful tool that enhances patient safety and medication management in healthcare settings. By leveraging barcodes and technology, BCMA reduces medication errors, enhances documentation accuracy, and provides decision support to healthcare professionals. Successful BCMA implementation requires careful planning, staff training, and integration with existing healthcare systems. While challenges exist, ongoing advancements and innovations in BCMA promise to further improve patient safety and healthcare outcomes.
FAQs (Frequently Asked Questions)
1. Does BCMA eliminate all medication errors? BCMA significantly reduces medication errors, but it cannot eliminate them entirely. It serves as an important safety measure by verifying medication and patient identity, but human factors and system limitations can still contribute to errors.
2. Can BCMA be implemented in all healthcare settings? BCMA can be implemented in various healthcare settings, including hospitals, long-term care facilities, and outpatient clinics. However, the specific requirements and considerations may vary depending on the setting’s size, complexity, and resources.
3. How does BCMA benefit healthcare providers? BCMA benefits healthcare providers by improving medication safety, reducing documentation errors, supporting clinical decision-making, and facilitating accurate medication reconciliation. It streamlines workflow processes and enhances the overall efficiency of medication administration.
4. Is BCMA compatible with existing electronic health record systems? Yes, BCMA can be integrated with existing electronic health record (EHR) systems. Integration allows for seamless data exchange, real-time access to patient information, and automatic documentation of medication administration.
5. How does BCMA impact patient outcomes? BCMA has a positive impact on patient outcomes by reducing medication errors, preventing adverse drug events, and improving medication adherence. It enhances patient safety and contributes to the delivery of high-quality care.
What are the five important steps of bar coded medication administration?
The five important steps of Bar Code Medication Administration (BCMA) are as follows:
- Verification of Medication: The first step involves scanning the barcode on the medication packaging to ensure that it matches the medication order in the electronic health record (EHR). This verification confirms that the right medication is being administered to the patient.
- Verification of Patient Identity: The second step is to scan the barcode on the patient’s identification wristband. This step ensures that the medication is being administered to the correct patient. It helps prevent medication errors due to patient misidentification.
- Verification of Medication Administration Time: Before administering the medication, the healthcare professional scans the barcode on the patient’s wristband and the medication packaging again. This step confirms that it is the right time to administer the medication, as per the prescribed schedule.
- Documentation of Medication Administration: After administering the medication, the healthcare professional scans the barcode on the medication packaging once more to document the administration in the patient’s electronic medication administration record (eMAR). This step ensures accurate and real-time documentation of medication administration.
- Real-Time Clinical Decision Support: Throughout the medication administration process, the BCMA system provides real-time clinical decision support. It alerts healthcare professionals to potential drug interactions, allergies, or other important information relevant to the medication being administered. This step helps healthcare providers make informed decisions and enhances patient safety.
What is the effect of the implementation of barcode technology and an electronic medication administration record on adverse drug events?
The implementation of barcode technology and an electronic medication administration record (eMAR) has a significant positive effect on reducing adverse drug events (ADEs).
Barcode technology allows for the accurate identification and verification of medications, patients, and healthcare providers. By scanning the barcodes on medication packaging, patient identification wristbands, and healthcare professionals’ identification badges, the system ensures that the right medication is being administered to the right patient. This verification process greatly reduces the risk of medication errors, such as administering the wrong medication, wrong dose, or wrong route.
The electronic medication administration record (eMAR) complements barcode technology by providing a digital record of medication administration. It captures real-time data regarding the administration of medications, including the time, dosage, and healthcare professional responsible. This electronic documentation is more accurate and reliable compared to traditional paper-based records, reducing the chances of errors or omissions.
The combination of barcode technology and eMAR enhances medication safety in several ways:
- Reduction in Medication Administration Errors: Barcode scanning ensures that the medication being administered matches the medication order in the electronic system, reducing the risk of administration errors. This accuracy significantly decreases the occurrence of ADEs caused by incorrect medication administration.
- Identification of Drug Interactions and Allergies: The electronic system can be integrated with clinical decision support tools that provide alerts for potential drug interactions and patient allergies. These alerts prompt healthcare professionals to exercise caution and make informed decisions, preventing ADEs related to medication interactions or known allergies.
- Real-Time Documentation and Monitoring: The eMAR allows for real-time documentation of medication administration. This immediate documentation improves accuracy and completeness, providing a clear overview of medications administered, dosages, and frequencies. It enables healthcare professionals to monitor medication regimens more effectively, reducing the likelihood of medication errors and potential ADEs.
- Data Analysis and Quality Improvement: The digital nature of eMAR facilitates data analysis for quality improvement initiatives. By analyzing medication administration data, healthcare organizations can identify patterns, trends, and potential areas for improvement. This proactive approach helps prevent ADEs and enhances patient safety.
Is implementing barcode medication administration and smart infusion pumps is just the beginning of the safety journey to prevent administration errors?
Implementing barcode medication administration (BCMA) and smart infusion pumps is indeed an essential step in the journey to prevent medication administration errors. However, it is important to recognize that it is just the beginning of the safety journey, and additional measures are required to comprehensively address medication administration errors.
Barcode medication administration, with its verification processes and documentation capabilities, significantly reduces the risk of errors related to medication identification and administration. Smart infusion pumps provide advanced features such as dose-rate calculations, drug libraries, and safety alerts, further enhancing the safety of intravenous medication administration. These technologies serve as crucial safeguards in preventing errors and improving patient safety.
However, it is essential to adopt a multi-faceted approach to medication safety that encompasses various aspects. Here are some additional measures that should be considered:
- Standardization of Medication Practices: Implementing standardized medication practices, such as the use of pre-mixed medications, unit-dose packaging, and clear labeling, helps reduce the likelihood of errors. Standardization promotes consistency, clarity, and ease of use for healthcare professionals.
- Robust Medication Reconciliation: Accurate medication reconciliation is crucial during transitions of care. Healthcare providers should ensure that the medication list is accurately maintained, and any discrepancies are addressed promptly. This process helps prevent errors stemming from incorrect medication orders or omissions.
- Comprehensive Staff Training and Education: Adequate training and education programs are vital for healthcare professionals to understand and utilize the technology effectively. Training should cover the use of barcode scanners, smart infusion pumps, and associated protocols. Continuous education ensures that staff members stay updated on best practices and any advancements in medication safety.
- Culture of Safety and Reporting: Fostering a culture of safety encourages healthcare professionals to report near-miss events, medication errors, and potential hazards without fear of retribution. Establishing mechanisms for reporting, investigating, and learning from errors is crucial for continuous improvement and preventing future incidents.
- Ongoing Evaluation and Improvement: Regular evaluation of medication safety practices is essential to identify areas for improvement. This can involve analyzing medication error reports, conducting audits, and implementing strategies to address identified issues. Continuous quality improvement initiatives help refine processes and enhance patient safety.
